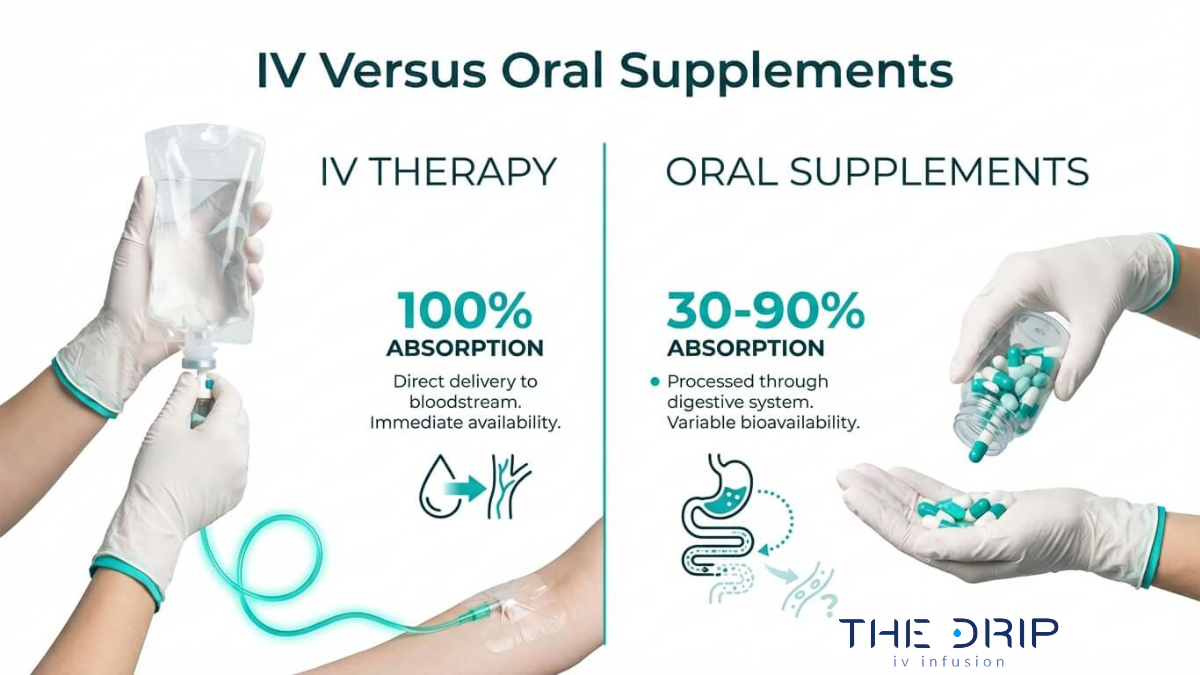
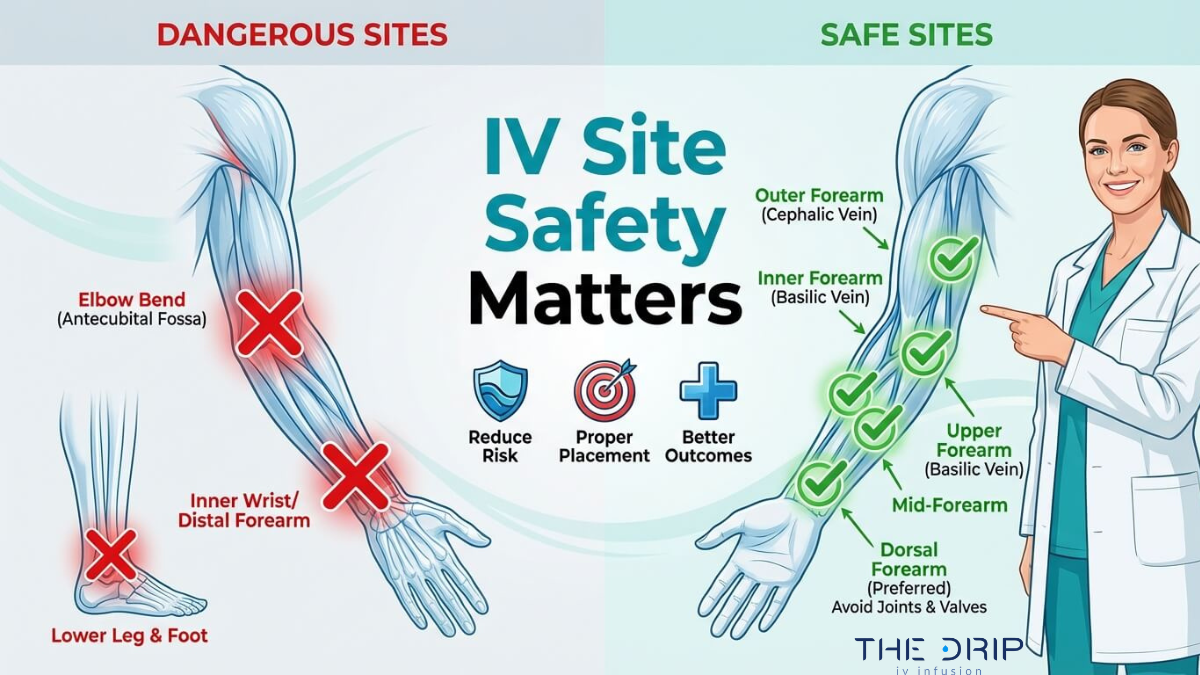
IV sites to avoid are specific anatomical locations and compromised veins where catheter insertion carries elevated risk of failure, infection, or tissue damage. These include areas of joint flexion, the inner wrist, lower extremities in adults, and limbs affected by mastectomy or AV fistulas.
This guide covers anatomical sites that demand avoidance, vein characteristics that signal poor access, patient conditions that restrict site options, complications caused by wrong-site placement, and how professional nursing protocols ensure safe IV insertion.
Certain body locations create mechanical and infection risks that outweigh their apparent convenience. The antecubital fossa, inner wrist, and lower leg veins each present distinct hazards ranging from catheter kinking and nerve injury to thrombosis and elevated bacterial colonization.
Vein quality matters as much as location. Thin, fragile, sclerosed, or bifurcated veins resist proper catheter threading and rupture more easily, increasing infiltration and extravasation risk during infusion.
Underlying health conditions further narrow safe options. Diabetic patients face higher IV access complication rates due to vessel damage and skin changes, while elderly patients present fragile venous walls that demand smaller gauges and slower infusion rates. Pediatric and pregnant patients each require tailored site strategies based on vessel size and thrombosis risk.
Wrong-site placement leads to measurable consequences, including phlebitis, infiltration, thrombophlebitis, and catheter-related bloodstream infections. Understanding these outcomes reinforces why site selection is a clinical skill, not a convenience choice.
Professional mobile IV therapy from The Drip IV Infusion applies these principles through trained nursing assessment, real-time monitoring, and adherence to evidence-based vein selection protocols during every at-home infusion session.
Which IV Insertion Sites Should Always Be Avoided?
Certain anatomical locations and clinical scenarios make IV insertion unsafe or significantly increase complication risk. The following subsections cover specific sites to avoid, from the antecubital fossa and inner wrist to extremities affected by surgery, infection, or injury.
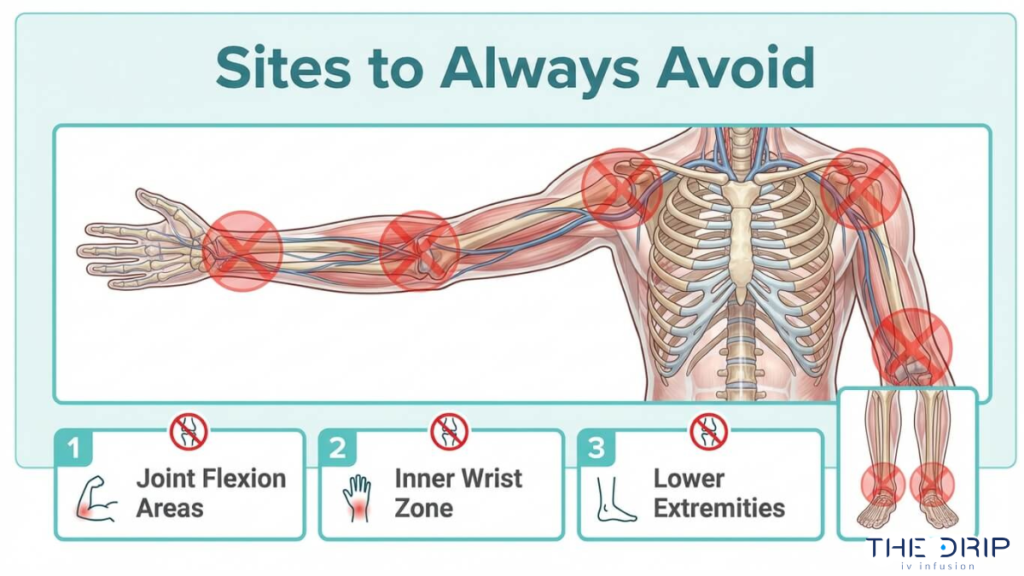
Why Should You Avoid IV Placement in the Antecubital Fossa?
You should avoid IV placement in the antecubital fossa because this bend-of-the-elbow site significantly increases catheter failure risk. Arm flexion at the elbow kinks the catheter, disrupting flow and causing mechanical irritation to the vein wall. According to a multivariate analysis published in Infection Control & Hospital Epidemiology, modifiable risks for accidental catheter removal include insertion in the antecubital fossa, hand, or upper arm compared with the forearm. The cubital fossa also carries elevated risk of catheter colonization and local infection. While the veins here appear large and inviting, particularly the median cubital vein, the constant joint movement makes this site unreliable for anything beyond a brief blood draw.
Why Is the Inner Wrist a Dangerous IV Site?
The inner wrist is a dangerous IV site because superficial nerves and tendons run immediately beneath the skin in this area. The radial and median nerves sit close to the palmar wrist veins, making needle insertion likely to cause sharp, shooting pain or nerve injury. The Infusion Nurses Society recommends avoiding the inner two-inch area of the wrist when starting an IV or drawing labs to prevent shocking the nerve. Tendon damage is another concern, since even minor catheter movement can irritate surrounding structures in this tightly packed anatomical zone. For most patients, the mid-forearm offers safer, more stable venous access with far less neurological risk.
Why Should IV Lines Avoid Areas of Joint Flexion?
IV lines should avoid areas of joint flexion because movement at the joint dislodges or occludes the catheter. According to The Royal Children’s Hospital Melbourne clinical guidelines, cannulas inserted over joints, in areas of flexion, or in the lower limb are more likely to fail than those inserted in the hand or forearm. Repeated bending compresses the catheter lumen, interrupts infusion flow, and irritates the vein lining. Patients with diabetes face additional challenges, as clinicians should avoid areas of lipohypertrophy or thickened skin that further compromise catheter stability. When prolonged therapy is anticipated, alternatives such as midline catheters or PICC lines placed in straighter vein segments offer better outcomes.
Why Is IV Insertion Near a Previous Infiltration Risky?
IV insertion near a previous infiltration site is risky because the surrounding tissue and vein wall are already compromised. Infiltration occurs when IV fluid leaks into the tissue outside the vein, causing swelling, tenderness, and localized damage. Reinserting a catheter near this area increases the chance of repeated infiltration, since the weakened vein wall may not hold the catheter securely. The swollen tissue also makes accurate vein visualization difficult, raising the likelihood of a failed attempt. Selecting a site above or on a different vein altogether gives the damaged area time to heal and provides a structurally sound vessel for reliable access.
Why Should You Avoid Starting an IV in the Lower Extremities?
You should avoid starting an IV in the lower extremities because veins in the legs and feet carry substantially higher risks of thrombosis and infection in adult patients. Reduced blood flow velocity in the lower limbs promotes clot formation around the catheter tip. The CDC recommends replacing any catheter inserted in a lower extremity site to an upper extremity site as soon as possible in adult patients. Pedal and saphenous veins are also more difficult to stabilize, and patient mobility further increases dislodgement risk. Pediatric patients represent an exception; according to the World Health Organization, the upper or lower extremities and the scalp in neonates can serve as catheter insertion sites when upper-body access is unavailable.
Why Is the Affected Side After Mastectomy an IV Site to Avoid?
The affected side after mastectomy is an IV site to avoid because lymph node removal disrupts normal lymphatic drainage, making that arm highly vulnerable to infection and lymphedema. According to the Anesthesia Patient Safety Foundation, clinical policies reinforce avoiding IV insertion, blood draws, or blood pressure cuff use on the affected arm post-mastectomy to reduce infection-related lymphedema risk. Even minor venous trauma from catheter placement can trigger swelling that becomes chronic. This restriction applies indefinitely, not just during the immediate recovery period. Clinicians should always ask patients about surgical history before selecting an IV site; the contralateral arm or an alternative upper-body vein provides much safer access.
Why Should IV Placement Be Avoided on an AV Fistula Arm?
IV placement should be avoided on an AV fistula arm because venous puncture can damage the fistula and compromise its maturation for hemodialysis access. An arteriovenous fistula is a surgically created connection between an artery and vein, and it requires uninterrupted blood flow to develop properly. Catheter insertion, blood draws, or tourniquets on this arm risk thrombosis, stenosis, or infection that could render the fistula unusable. For patients with advanced kidney disease, the subclavian site should also be avoided to prevent subclavian vein stenosis, according to guidelines published in Infection Control & Hospital Epidemiology. Protecting vascular access for dialysis is a clinical priority that overrides convenience in site selection.
Why Are Areas With Active Infection Unsafe for IV Access?
Areas with active infection are unsafe for IV access because inserting a catheter through infected skin introduces bacteria directly into the bloodstream. This creates a pathway for systemic infection, including bacteremia and sepsis. A study published in the Journal of Family Medicine and Primary Care found that local complications at IV access sites occur in more than 50% of patients, with phlebitis at 21.6% and infiltration at 14% being the most common. Placing a catheter near cellulitis, abscess, or any visibly inflamed tissue dramatically amplifies these rates. The femoral vein should similarly be avoided for central venous access in adults due to higher colonization rates. Clinicians must select a site with intact, healthy skin.
Why Should You Avoid IV Insertion in Edematous Extremities?
You should avoid IV insertion in edematous extremities because excess fluid in swollen tissue obscures vein visibility and compromises catheter placement accuracy. Edema stretches the skin and compresses superficial veins, making palpation unreliable and increasing failed insertion attempts. Even when a catheter is successfully placed, the surrounding tissue pressure can slow infusion rates and promote infiltration as fluid leaks into already overloaded compartments. Swollen extremities also signal underlying circulatory compromise, meaning the veins themselves may be fragile or poorly perfused. Choosing a non-edematous limb, or using ultrasound guidance to locate deeper viable veins, produces safer and more reliable intravenous access.
Why Is Placing an IV Near Burned or Injured Skin Prohibited?
Placing an IV near burned or injured skin is prohibited because damaged tissue lacks the structural integrity and infection resistance needed for safe catheter placement. According to the Merck Manual Professional Version, contraindications for peripheral intravenous catheter insertion include infection or burned skin at a prospective cannulation site, an injured or massively edematous extremity, or a thrombotic or phlebitic vein. Burn injuries destroy the skin’s protective barrier, and inserting a needle through compromised tissue dramatically increases bacterial entry risk. Injured veins beneath traumatized skin may also be partially thrombosed or structurally weakened. Understanding which sites demand avoidance helps clinicians select access points that support both safety and treatment success.
What Vein Characteristics Make an IV Site Unsuitable?
Certain vein characteristics make an IV site unsuitable because they increase catheter failure, infiltration, and patient discomfort. The sections below cover small or fragile veins, sclerosed veins, bifurcated veins, and previously phlebotomized veins.
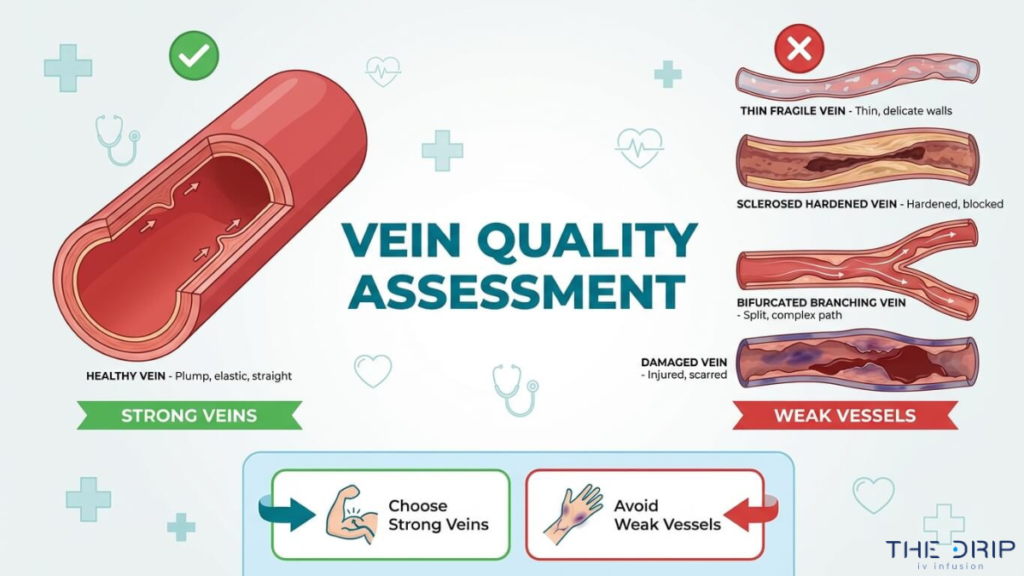
Why Should Small or Fragile Veins Be Avoided for IV Access?
Small or fragile veins should be avoided for IV access because they rupture easily during catheter insertion, leading to infiltration and failed lines. According to a study published in the Journal of Clinical Nursing, the most frequent abnormal vessel characteristics complicating IV access are thin veins (19.4%), fragile veins (14.5%), tortuous veins (13.6%), and hard veins (13.6%). Fragile veins lack the structural integrity to withstand catheter movement or fluid pressure, making them especially problematic for sustained infusions. Elderly patients and individuals with chronic conditions often present with these vein types, requiring clinicians to identify stronger, more resilient alternatives before attempting access.
Why Are Sclerosed or Hardened Veins Poor IV Choices?
Sclerosed or hardened veins are poor IV choices because their rigid, fibrotic walls resist catheter advancement and prevent proper blood return. Sclerosis occurs when repeated venipuncture, irritating medications, or chronic IV use causes the vein wall to thicken and lose elasticity. A catheter forced into a sclerosed vein often fails to thread correctly, increasing the risk of infiltration or extravasation. These veins also feel cord-like on palpation, which may seem like a visible target but actually signals compromised vascular tissue unsuitable for infusion. Clinicians should bypass sclerosed segments entirely and select a softer, more pliable vein to ensure reliable catheter placement.
Why Should Bifurcated or Branching Veins Be Avoided?
Bifurcated or branching veins should be avoided because the junction where a vein splits creates a natural obstruction point for catheter tips. When a catheter reaches a bifurcation, it can press against the vessel wall at the branch point, causing mechanical irritation, reduced flow rates, or vessel perforation. Valves often cluster near these junctions, further impeding smooth catheter threading. Attempting insertion at or just above a bifurcation increases the likelihood of positional malfunction, where the catheter works only in certain arm positions. Selecting a straight, unbranched vein segment gives the catheter a clear path and reduces the risk of flow interruption during the infusion.
Why Are Previously Phlebotomized Veins Risky for IV Starts?
Previously phlebotomized veins are risky for IV starts because recent puncture sites create weak points in the vessel wall where fluid can leak into surrounding tissue. Inserting a catheter at or near a fresh venipuncture wound compromises the vein’s structural integrity, increasing infiltration risk. Repeated draws from the same vein also promote localized inflammation and early-stage sclerosis, further degrading the vessel’s suitability for sustained infusion. Best practice is to select a site proximal to any recent puncture or choose an entirely different vein. Understanding how vein condition shapes IV outcomes helps explain why certain patient populations face additional site restrictions.
Why Do Certain Patient Conditions Limit IV Site Selection?
Certain patient conditions limit IV site selection because underlying health factors alter vein integrity, skin quality, and complication risk. The following subsections cover site restrictions for diabetic, elderly, pediatric, pregnant, and anticoagulated patients.
Which IV Sites Should Be Avoided in Diabetic Patients?
The IV sites that should be avoided in diabetic patients include areas of lipohypertrophy, thickened skin, and lower extremities where peripheral neuropathy reduces sensation. Diabetes damages small blood vessels over time, making veins harder to access and more prone to failure. A 2021 study published in the Journal of Family Medicine and Primary Care found that IV access complications are significantly more prevalent in diabetic patients (p = 0.0003) compared to non-diabetics. Clinicians should target well-visible forearm veins and avoid sites where tissue changes mask early signs of infiltration. For diabetic patients receiving any infusion, careful vein assessment before insertion is arguably the single most important step in preventing complications.
Which IV Sites Should Be Avoided in Elderly Patients?
The IV sites that should be avoided in elderly patients include the dorsal hand veins, areas over bony prominences, and any site with visibly fragile or rolling veins. Aging thins the venous walls and reduces subcutaneous tissue support, which increases the risk of infiltration and hematoma formation. According to the Open RN Nursing Skills textbook, older adults have delicate venous walls that may not withstand rapid infusion rates, requiring frequent monitoring for fluid volume overload and site patency. Selecting a straight, well-supported forearm vein with the smallest effective catheter gauge minimizes trauma. Gentle anchoring and slower infusion rates further protect these vulnerable vessels.
Which IV Sites Should Be Avoided in Pediatric Patients?
The IV sites that should be avoided in pediatric patients include the dominant hand, areas near joints where movement causes dislodgement, and foot veins in ambulatory children. Small vessel diameter and limited cooperation make site selection especially critical. The World Health Organization notes that in pediatric patients, the upper or lower extremities or the scalp in neonates and young infants can be used as catheter insertion sites. Scalp veins are reserved for neonates when extremity access fails. Securing the catheter properly is essential because children move unpredictably, and even well-placed lines dislodge easily without adequate stabilization.
Which IV Sites Should Be Avoided During Pregnancy?
The IV sites that should be avoided during pregnancy include the antecubital fossa on the dominant arm, lower extremity veins, and any site prone to positional occlusion. Pregnant patients often experience increased blood volume and mild peripheral edema, which can obscure vein landmarks while also raising the risk of deep vein thrombosis in the legs. The CDC recommends replacing any catheter inserted in a lower extremity to an upper extremity site as soon as possible in adult patients, a guideline that carries particular weight during pregnancy. The non-dominant forearm provides the most stable, comfortable access point during labor and prenatal hydration sessions.
Which IV Sites Should Be Avoided in Patients on Blood Thinners?
The IV sites that should be avoided in patients on blood thinners include deep veins, areas with limited visibility, and any location where applying adequate pressure after removal would be difficult. Anticoagulant medications like warfarin and heparin impair clot formation, so even minor vessel trauma during cannulation can produce significant hematomas. Selecting a superficial, straight forearm vein allows direct visualization and easy compression post-procedure. Clinicians should also avoid multiple insertion attempts because each failed stick creates an additional bleeding site. For patients on blood thinners, the margin for error in site selection narrows considerably, making precise first-attempt placement a clinical priority rather than a preference.
With patient-specific restrictions addressed, understanding what happens when an IV is placed incorrectly highlights why these precautions matter.
What Happens When an IV Is Placed in the Wrong Site?
Placing an IV in the wrong site causes complications ranging from mild swelling to serious tissue damage and systemic infection. The most common consequences include infiltration, extravasation, phlebitis, thrombosis, and catheter-related bloodstream infections.

What Is IV Infiltration and How Does a Wrong Site Cause It?
IV infiltration is the leakage of non-vesicant fluid from the catheter into surrounding tissue instead of entering the vein. A wrong site causes infiltration when the catheter punctures through or dislodges from a fragile, poorly anchored, or overly mobile vein. Sites near joints or in areas of flexion increase catheter movement, raising the likelihood of this complication. According to a 2024 large-scale clinical study published in PMC (Kaphan et al.), phlebitis occurred at 2.41% of all IV sites while infiltration occurred at 1.01%. Even at relatively low incidence rates, infiltration causes localized swelling, pain, and coolness at the site, potentially delaying treatment.
What Is IV Extravasation and Why Is It a Serious Complication?
IV extravasation is the leakage of vesicant (tissue-damaging) medication from a catheter into surrounding tissue. This complication is serious because vesicant solutions can cause blistering, tissue necrosis, and permanent damage that may require surgical intervention. Extravasation occurs more frequently when catheters are placed in unstable sites with poor vein integrity. Unlike standard infiltration, the severity depends on the caustic nature of the infused medication. For this reason, clinicians reserve vesicant infusions for well-secured, properly positioned IV lines in healthy, stable veins.
How Does a Poor IV Site Lead to Phlebitis?
A poor IV site leads to phlebitis by creating mechanical irritation against the vein wall. When a catheter is placed in a small, superficial, or frequently flexing vein, repeated friction triggers inflammation of the vessel lining. Symptoms include redness, warmth, tenderness, and a palpable cord along the vein. As noted in a study published in International Emergency Nursing, “poorly managed PIVCs can create portals for infection and a source of ongoing discomfort for patients, leading to complications and patient dissatisfaction.” Choosing appropriately sized veins in stable anatomical locations significantly reduces phlebitis risk.
Can a Bad IV Site Cause a Blood Clot or Thrombosis?
Yes, a bad IV site can cause a blood clot or thrombosis. Thrombophlebitis is the inflammation of a vein in conjunction with the formation of a blood clot, or thrombus. Poorly selected IV sites accelerate this process because mechanical irritation from the catheter damages the vein’s endothelial lining, activating the clotting cascade. Veins that are already compromised, too small for the catheter gauge, or located in high-movement areas are particularly vulnerable. Once a thrombus forms, it can obstruct blood flow, cause significant pain, and in rare cases contribute to more serious vascular events if left unaddressed.
How Does Wrong Site Selection Increase Infection Risk?
Wrong site selection increases infection risk by placing catheters in areas with higher bacterial colonization or compromised skin integrity. Sites near the groin, lower extremities, or damaged skin harbor more microorganisms, creating a direct pathway for pathogens to enter the bloodstream. According to a randomized controlled trial published in Infection Control & Hospital Epidemiology, catheter failure risk factors include site location, reinforcing that clinical assessment of a site’s integrity matters more than arbitrary rotation schedules. Rotating IV sites based on clinical evaluation every 72 to 96 hours, rather than fixed schedules alone, helps minimize colonization and reduces catheter-related bloodstream infections.
Understanding these complications reinforces why proper site selection is foundational to safe IV therapy.
What Are the Best IV Sites to Use Instead?
The best IV sites to use instead are the veins of the forearm, the dorsal hand, and, when clinically appropriate, the upper arm. These locations balance vein accessibility, patient comfort, and lower complication risk. The following subsections cover each preferred site and why it works well.
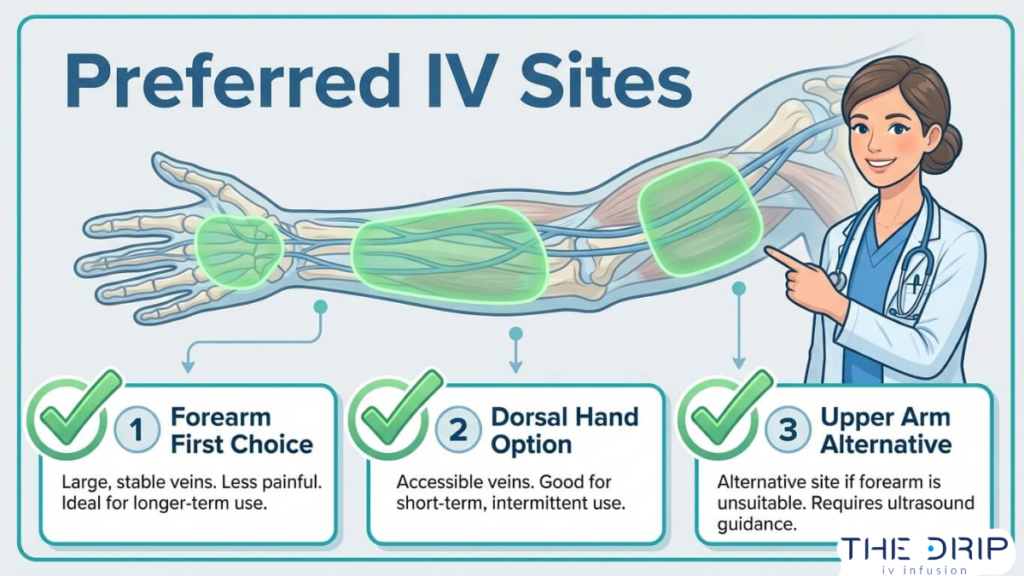
Why Is the Forearm the Preferred IV Site?
The forearm is the preferred IV site because it offers straight, well-supported veins with minimal joint movement. Veins like the cephalic and basilic veins in this region sit over a stable surface of muscle and bone, reducing the risk of catheter dislodgement. According to a study published in Infection Control & Hospital Epidemiology, insertion in the antecubital fossa, hand, or upper arm carries higher modifiable risk for accidental removal compared with the forearm. Clinically, this makes the mid-forearm the safest default for most peripheral IV starts. For patients needing extended infusion sessions, the forearm’s stability also helps maintain consistent flow rates with fewer interruptions.
When Is the Dorsal Hand a Good IV Option?
The dorsal hand is a good IV option when forearm veins are inaccessible or when short-duration infusions are planned. Superficial veins on the back of the hand, such as the dorsal metacarpal veins, are visible and easy to palpate in most patients. These veins work well for single-session therapies where the catheter will not remain in place for extended periods. However, hand placement does involve more movement at the wrist, so proper stabilization with a securement device is essential. For most wellness-focused IV sessions lasting around one hour, the dorsal hand provides reliable access with minimal discomfort.
Why Is the Upper Arm Used as an Alternative IV Site?
The upper arm is used as an alternative IV site when forearm and hand veins are not viable. The basilic vein in the upper arm provides a large-caliber option that accommodates higher flow rates. This site is particularly useful for patients with difficult venous access, such as those with thin or fragile veins. According to a study in the Journal of Clinical Nursing, the most frequent abnormal vessel characteristics complicating IV access are thin veins (19.4%), fragile veins (14.5%), and tortuous veins (13.6%). In these cases, the upper arm’s deeper, larger veins offer a practical alternative. Proper assessment remains critical, since upper arm placement can limit mobility more than forearm sites.
With preferred sites identified, understanding how nurses evaluate and select among them ensures the safest possible IV placement.
How Do Nurses Choose a Safe IV Insertion Site?
Nurses choose a safe IV insertion site by assessing vein quality, patient history, and treatment requirements before placing a catheter. The subsections below cover the clinical assessment process, the role of ultrasound technology, and site rotation protocols.
How Do Nurses Assess Vein Quality Before IV Insertion?
Nurses assess vein quality before IV insertion by visually inspecting and palpating the arm to evaluate vein size, resilience, and straightness. A bouncy, well-anchored vein in the forearm is typically preferred over veins that feel hard, rolling, or cord-like. According to a study published in the Journal of Clinical Nursing, the most frequent abnormal vessel characteristics complicating IV access are thin veins (19.4%), fragile veins (14.5%), and tortuous or hardened veins (13.6% each). Patient factors such as hydration status, medication use, and prior IV history also shape the nurse’s assessment. Experienced nurses often apply a tourniquet and ask patients to make a fist, which engorges veins and makes selection more reliable. This systematic evaluation is what separates a smooth, first-attempt insertion from repeated, uncomfortable needle sticks.
How Does Ultrasound Help Nurses Find Safe IV Sites?
Ultrasound helps nurses find safe IV sites by providing real-time visualization of vein depth, diameter, and surrounding structures beneath the skin. This technology is especially valuable for patients with difficult venous access, such as those with obesity, chronic illness, or a history of IV drug use, where surface veins are not visible or palpable. According to the Journal of the Association for Vascular Access, real-time ultrasound guidance for peripheral IV placement reduces mechanical complications and the number of attempts required. With ultrasound, nurses can distinguish veins from arteries, identify thrombosed segments, and select a vessel with adequate caliber for the prescribed therapy. For patients who have experienced multiple failed sticks, ultrasound-guided insertion is one of the most effective tools available.
Why Is IV Site Rotation Important for Patient Safety?
IV site rotation is important for patient safety because leaving a catheter in one location too long increases the risk of phlebitis, infiltration, and catheter-related infection. Clinical protocols typically call for reassessing IV sites regularly and rotating them based on the condition of the vein and surrounding tissue. Each clinician should also limit insertion attempts; The Royal Children’s Hospital Melbourne recommends a maximum of two attempts per clinician before escalating to a more experienced provider or using ultrasound assistance. Rotation preserves vein integrity across the vascular network, ensuring that future IV access remains available when needed. For patients requiring ongoing infusions, this disciplined approach to site management directly reduces complications and discomfort over time.
Understanding how nurses select and maintain safe IV sites highlights the value of professional oversight during any infusion.
How Does Professional Mobile IV Therapy Ensure Safe IV Placement?
Professional mobile IV therapy ensures safe IV placement through trained nursing protocols, proper site selection, and continuous monitoring throughout the infusion. The following sections cover how nurse-administered infusions reduce complications and summarize key takeaways about IV sites to avoid.
Can Nurse-Administered Mobile IV Infusions From The Drip IV Infusion Reduce IV Site Complications?
Yes, nurse-administered mobile IV infusions from The Drip IV Infusion can reduce IV site complications through expert vein assessment and adherence to clinical protocols. Common patient concerns include risks of infiltration, extravasation, and phlebitis during home infusions, and trained nurses address each of these through careful site selection and real-time monitoring.
As noted in the Nursing Skills open textbook, “Careful site selection is crucial to ensuring the success and longevity of IV access. By choosing the appropriate site, we can reduce complications, enhance patient comfort, and improve overall outcomes.”
The Drip IV Infusion applies these principles during every session by:
- Evaluating vein health before selecting an insertion site, avoiding compromised or fragile vessels.
- Adjusting infusion rates for vulnerable populations, since older adults have delicate venous walls that may not withstand rapid delivery.
- Monitoring site patency and fluid volume throughout the one-hour session.
This hands-on nursing approach makes professional mobile IV therapy a safer alternative to unmonitored infusion setups.
What Are the Key Takeaways About IV Sites to Avoid?
The key takeaways about IV sites to avoid center on three principles: anatomical awareness, patient-specific restrictions, and vein quality assessment. Certain locations, such as areas of joint flexion, the inner wrist, lower extremities, and limbs affected by mastectomy or AV fistulas, carry elevated complication risks. Patient conditions including diabetes, advanced age, and pregnancy further narrow safe options.
According to a large-scale clinical review, vein irritation was reported in approximately 2–3% of IV sites, while fluid leakage under the skin occurred in about 1%. These rates remain low when qualified professionals select appropriate veins and avoid known contraindicated sites.
Prioritizing proper IV site selection is one of the simplest ways to prevent complications. The Drip IV Infusion brings this clinical expertise directly to clients, combining professional nursing skill with the convenience of at-home infusions.