IV therapy administration is a legally regulated medical procedure that only licensed healthcare professionals can perform. The specific providers authorized, and the rules governing their practice, depend on state-level scope-of-practice laws, supervision mandates, and certification requirements.
This guide covers licensed provider categories and their authority levels, education and certification pathways, state regulatory frameworks, clinical versus mobile delivery settings, and provider evaluation criteria.
Physicians hold the broadest independent authority to order and perform IV therapy, while registered nurses serve as the most common professionals physically starting lines and managing infusions. Licensed practical nurses, paramedics, physician assistants, nurse practitioners, and certified registered nurse anesthetists each operate under distinct scope limitations that vary by jurisdiction.
Qualifying to administer IV therapy requires accredited clinical education, state licensure, and in many cases post-licensure IV training with competency verification. Voluntary credentials like the CRNI® and VA-BC™ validate advanced infusion and vascular access expertise beyond baseline licensing.
State nursing boards, medical boards, and pharmacy boards each regulate different aspects of IV therapy practice, yet no single national standard governs these services. This regulatory patchwork means provider authorization recognized in one state may not transfer to another, making local verification essential.
The clinical setting shapes staffing and oversight structure. Hospital and clinic environments maintain institutional protocols and on-site medical teams, while mobile services send licensed RNs directly to homes, offices, and events with the same professional credentials. Choosing a qualified provider requires confirming active licensure, checking for specialty certifications, and evaluating standardized safety protocols covering sterile technique, patient screening, and emergency preparedness.
What Healthcare Professionals Are Licensed to Administer IV Therapy?
The healthcare professionals licensed to administer IV therapy include physicians, registered nurses, licensed practical nurses, paramedics, physician assistants, nurse practitioners, and certified registered nurse anesthetists. Each provider type operates under distinct scope-of-practice rules shaped by state law.
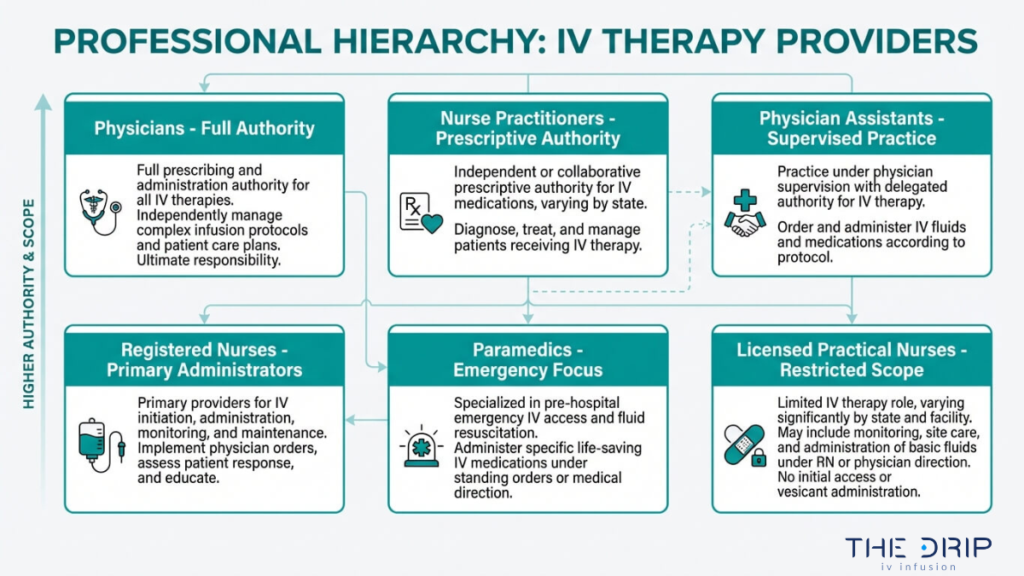
Physicians
Physicians hold the broadest authority to administer IV therapy. As licensed medical doctors (MDs) or doctors of osteopathic medicine (DOs), physicians can independently order, prescribe, and perform intravenous treatments without supervisory requirements. Their prescriptive authority also enables them to authorize other licensed professionals to carry out IV administration on their behalf. In Arizona, for example, a valid medical order from a licensed provider with prescriptive authority is required before an LPN or RN can administer IV fluids, nutrient therapies, or medications. Physicians serve as the foundational link in the IV therapy chain of command, making their role essential even when they are not the ones physically starting the line.
Registered Nurses
Registered nurses are the most common professionals who physically administer IV therapy. RNs complete extensive clinical training in venipuncture, fluid management, and infusion monitoring as part of their nursing education. Their scope of practice in most states permits them to initiate peripheral IV lines, administer prescribed fluids and medications, and monitor patients throughout the infusion process. This hands-on role makes RNs the backbone of both clinical and mobile IV services. For practitioners prioritizing patient safety, an RN’s combination of assessment skills and infusion competency is difficult to match among other provider types.
Licensed Practical Nurses
Licensed practical nurses may administer IV therapy, but their scope is more restricted than that of registered nurses. Most states require LPN/LVNs to complete a post-licensure IV education course and pass skill competency verification before they can practice IV therapy, according to Pedagogy Education. Several states impose additional limitations:
- New York permits LPNs to insert short peripheral IV catheters (3 to 6 cm) in superficial veins but prohibits midline catheters, long peripheral IV catheters, and central venous access devices.
- Missouri issues licenses explicitly stating “LPN IV-Certified” once board-approved requirements are met.
- Kansas prohibits any LPN from performing intravenous fluid therapy unless qualified under KSA 65-1136.
When a state requires LPN procedures to be performed “under supervision,” a registered nurse or physician must be physically present in the room during administration.
Paramedics and Emergency Medical Technicians
Paramedics and emergency medical technicians are trained in IV access, yet their authorization outside emergency settings remains limited. Most states prohibit paramedics from owning and operating independent IV hydration businesses because their scope of practice is typically restricted to emergency medical services under physician supervision, as noted by the Cohen Healthcare Law Group. Still, in some jurisdictions, EMTs or paramedics are among the few professionals, besides physicians and nurses, permitted to administer IV fluids in non-emergency settings. Anyone considering a paramedic-staffed IV service should verify that the provider’s state explicitly allows this practice beyond the ambulance.
Physician Assistants
Physician assistants are licensed to administer IV therapy under the supervision of a collaborating physician. PAs complete rigorous medical training that includes pharmacology, patient assessment, and procedural skills such as venous access. Their collaborative practice agreements typically grant them authority to order and administer IV fluids and medications. Because PAs practice medicine rather than nursing, their regulatory framework falls under state medical boards rather than nursing boards, which can affect how IV services are structured and overseen.
Nurse Practitioners
Nurse practitioners are advanced practice registered nurses with prescriptive authority who can both order and administer IV therapy. Some states require nurse practitioners to hold specific pharmacological certifications to practice IV infusion medicine due to the prescriptive authority involved in ordering treatments. In states that grant full practice authority, NPs can independently evaluate patients, prescribe IV formulations, and oversee infusion delivery without physician collaboration. This makes nurse practitioners particularly well suited for directing IV therapy services in wellness and outpatient settings.
Certified Registered Nurse Anesthetists
Certified registered nurse anesthetists are advanced practice nurses with extensive IV and vascular access expertise developed through anesthesia training. CRNAs routinely place peripheral and central lines, titrate IV medications, and manage fluid resuscitation in surgical and critical care environments. Nurses specializing in infusion can also pursue the CRNI credential; recertification requires an active, unrestricted RN license and at least 1,000 hours of infusion experience within the previous three-year certification cycle, according to the Infusion Nurses Certification Corporation. CRNAs represent some of the most technically skilled IV practitioners available, though they primarily work in procedural and hospital settings rather than elective wellness services.
Understanding which providers hold valid IV therapy credentials is the first step; the next consideration is what specific qualifications each professional must meet.
What Qualifications Are Required to Administer IV Therapy?
The qualifications required to administer IV therapy include specific educational degrees, professional certifications, and verified hands-on clinical training. The following subsections break down each requirement.
What Education and Degree Requirements Must Providers Meet?
The education and degree requirements providers must meet depend on their professional role. Registered nurses need an Associate Degree in Nursing (ADN) or a Bachelor of Science in Nursing (BSN), while licensed practical nurses must complete an accredited practical nursing program. Nurse practitioners and physician assistants require graduate-level education, typically a master’s or doctoral degree in their respective fields.
Each of these pathways includes foundational coursework in anatomy, pharmacology, and sterile technique. These subjects form the clinical knowledge base necessary for safe venipuncture, fluid administration, and patient monitoring during IV therapy. Without completing an accredited program, healthcare professionals cannot obtain the state licensure that authorizes IV administration.
What Certifications Are Needed for IV Therapy Administration?
The certifications needed for IV therapy administration vary by provider type and state. Most states require licensed practical nurses to complete a post-licensure IV education course and pass a skill competency verification before they can practice IV therapy. Nurse practitioners in certain states must hold specific pharmacological certifications due to the prescriptive authority involved in ordering IV treatments.
Beyond baseline licensure, voluntary credentials strengthen a provider’s qualifications:
- The Certified Registered Nurse Infusion (CRNI) credential validates advanced infusion expertise for registered nurses.
- The Vascular Access Board Certification (VA-BC) recognizes specialized competency in vascular access procedures.
These certifications signal a higher standard of training. For patients evaluating providers, asking about credentials beyond basic licensure is one of the most practical ways to assess clinical competency.
What Hands-On Training and Clinical Hours Are Necessary?
The hands-on training and clinical hours necessary for IV therapy certification combine supervised practice with classroom instruction. According to Florida Administrative Code 64B9-12.005, LPNs must complete at least 30 hours of post-graduation instruction covering both didactic coursework and clinical practice to earn IV therapy certification.
Clinical training typically includes:
- Peripheral venipuncture technique and catheter insertion
- IV fluid preparation and infusion rate calculation
- Adverse reaction recognition, including signs of infiltration and phlebitis
- Aseptic technique and infection prevention protocols
Didactic hours alone cannot prepare a provider for the real-world variability of patient veins, comfort levels, and potential complications. Supervised clinical practice bridges that gap, building the muscle memory and situational judgment that classroom learning cannot replicate.
With these qualifications established, the next question is whether specialized certification adds further value.
Do IV Therapy Providers Need Special Certification?
IV therapy providers benefit from special certifications that validate advanced competency in infusion and vascular access procedures. The two most recognized credentials are the CRNI® from the Infusion Nurses Society and the VA-BC™ from the Vascular Access Certification Corporation.
What Is the Infusion Nurses Society INS Certification?
The Infusion Nurses Society (INS) certification is a professional credential, designated as CRNI® (Certified Registered Nurse Infusion), that validates a registered nurse’s specialized expertise in infusion therapy practice. The Infusion Nurses Certification Corporation (INCC) administers this credential, which demonstrates proficiency across vascular access, pharmacology, and patient safety protocols.
Maintaining the CRNI® requires ongoing professional development. According to the Infusion Nurses Society, CRNI®s choosing to recertify by continuing education must obtain 40 Recertification Units during their 3-year cycle, with 30 of those RUs required to come from INS meetings or educational programming. This rigorous renewal process ensures that certified infusion nurses remain current with evolving best practices, making the CRNI® one of the strongest trust signals a patient can look for when evaluating an IV therapy provider.
What Is the Vascular Access Board Certification?
The Vascular Access Board Certification (VA-BC™) is a multidisciplinary credential recognizing clinical competency in vascular access device insertion, management, and care. The Vascular Access Certification Corporation (VACC) administers this certification.
Eligibility requirements include:
- A minimum of post-secondary education.
- At least one year of professional experience as a credentialed healthcare professional, such as an MD, PA, NP, RN, LPN, or EMT.
- Clinical practice involving vascular access procedures.
According to the VACC, VA-BC™ recertification requires either retaking the certification exam or earning 30 continuing education credits from vascular access-related sources over a three-year cycle. Certified clinicians are strictly prohibited from practicing outside their legal scope as defined by legislative or regulatory authority. For patients, this certification confirms that their provider has met standardized competency benchmarks specifically tied to safe venous access.
Does IV Certification Vary by State?
Yes, IV certification requirements vary by state. Each state’s board of nursing or medical board sets its own rules for which professionals can perform IV therapy and what additional training or certification they must complete. Some states mandate specific post-licensure IV courses before nurses can start peripheral lines, while others accept national certifications like the CRNI® or VA-BC™ as sufficient proof of competency.
This patchwork of regulations means a credential recognized in one state may not carry the same authority in another. Patients should verify that their IV therapy provider holds credentials aligned with their specific state’s licensing requirements, not just a national certification alone.
With certification standards clarified, understanding whether nurses can work independently during IV administration adds another important layer of provider evaluation.
Can Nurses Administer IV Therapy Without a Doctor Present?
Yes, nurses can administer IV therapy without a doctor present in many situations, though the specific rules depend on state regulations, the nurse’s license type, and whether a valid medical order is in place. The key factors include supervision requirements, standing orders, and scope-of-practice laws.
Registered nurses generally have the broadest authority among nursing professionals to perform IV therapy independently. In most states, an RN with demonstrated clinical competency can initiate and manage IV infusions once a licensed provider has issued the medical order. The provider does not necessarily need to be physically present during administration; the order itself serves as the authorizing directive.
Licensed practical nurses face stricter requirements. According to the Florida Hospital Association, when a state requires an LPN to perform procedures “under supervision,” a registered nurse or physician must be physically present in the room during administration. This distinction means LPNs often cannot work as independently as RNs in IV therapy settings.
The clinical stakes of unsupervised practice are real. A study published in the Journal of Vascular Access recorded 113 peripheral intravenous therapy infiltration/extravasation events from 3,476 catheters, representing an incidence rate of 3.25%. Complications like these underscore why proper training and appropriate oversight matter, regardless of whether a physician is on-site.
Several factors determine whether a nurse can administer IV therapy without direct physician presence:
- License type: RNs typically have broader independent authority than LPNs.
- State-specific scope of practice: Regulations vary significantly across jurisdictions.
- Valid medical order: A prescribing provider must authorize the treatment, even if not physically present.
- Clinical competency verification: The nurse must have completed required training and skill validation.
- Practice setting: Mobile, home-based, and wellness clinic settings may carry additional regulatory requirements.
For anyone considering IV therapy, the most important safety factor is not whether a physician stands in the room, but whether a qualified, licensed nurse operates under proper medical authorization with verified clinical skills. Understanding how state boards regulate these arrangements shapes the legal framework providers must follow.
What State Licensing and Regulatory Requirements Apply?
State licensing and regulatory requirements for IV therapy vary significantly across jurisdictions, affecting which professionals can practice and under what conditions. The following subsections cover the boards that regulate providers, scope-of-practice laws, and supervision mandates.
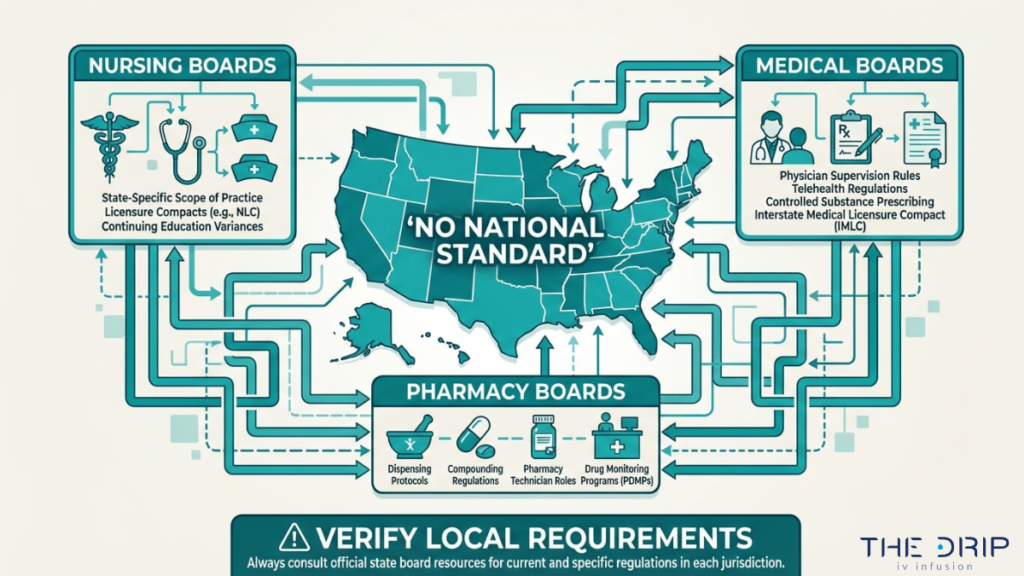
Which State Boards Regulate IV Therapy Providers?
State boards that regulate IV therapy providers include boards of nursing, boards of medicine, and boards of pharmacy, depending on the jurisdiction and the type of professional delivering treatment. No single national regulatory body oversees IV therapy administration.
State nursing boards typically govern RN and LPN scope of practice for infusion services. Boards of medicine regulate physician oversight requirements and prescriptive authority. According to the Oregon State Board of Nursing, IV hydration therapy may fall within the scope of practice of other healthcare professions, and questions about its administration should be directed to the relevant licensing boards. This means providers must check multiple regulatory bodies before offering IV services.
Because oversight is fragmented, practitioners should consult their specific state board to confirm which licenses and approvals apply to their practice setting.
What Scope-of-Practice Laws Govern IV Administration?
Scope-of-practice laws that govern IV administration define which clinical tasks each provider category can legally perform, including catheter insertion, fluid selection, and medication delivery. These laws are established at the state level through nursing practice acts, medical practice acts, and administrative codes.
Key elements that scope-of-practice laws typically address include:
- Which catheter types each provider level may insert.
- Whether a valid medical order from a licensed prescriber is required before administration.
- Which additives or medications fall within a provider’s authorized practice.
- Whether additional post-licensure IV education or competency verification is mandatory.
Scope boundaries carry strict enforcement. Clinicians in vascular access are prohibited from practicing outside their legal scope as defined by legislative or regulatory authority, with no exceptions for professional boundary violations. Providers who offer wellness IV services should verify that elective treatments fall within their state-defined scope.
What Supervision Requirements Exist for Different Providers?
Supervision requirements for different IV therapy providers range from fully independent practice for physicians to direct physical oversight for LPNs, depending on state regulations and provider credentials.
Physicians and certain advanced practice providers typically administer IV therapy independently. RNs generally practice under standing orders or protocols established by a prescribing provider. LPN supervision standards tend to be the most restrictive. According to a 2025 study published in the Journal of the American Medical Association, only 11.8% of U.S. states have issued specific position statements regarding the governance of IV hydration spas, with most focusing on the practice of medicine.
This regulatory gap means many IV therapy businesses operate without clear, standardized supervision guidelines. For consumers, verifying that a provider follows structured oversight protocols remains one of the most practical ways to ensure safe IV therapy administration.
Can Non-Medical Professionals Legally Administer IV Therapy?
Non-medical professionals cannot legally administer IV therapy in most states. Scope-of-practice laws restrict IV insertion and infusion to licensed healthcare providers operating under proper medical oversight.
Most states prohibit paramedics from owning and operating independent IV hydration businesses because their scope of practice is typically restricted to emergency medical services under physician supervision, according to the Cohen Healthcare Law Group. In some jurisdictions, EMTs or paramedics may be permitted to administer IV fluids in non-emergency settings, but only when specific state regulations allow it.
The Arkansas Department of Health emphasizes that IV therapy is a complex, learned skill requiring significant considerations for safe performance outside traditional medical facilities. This complexity is precisely why unlicensed individuals face legal consequences when attempting to offer these services independently.
Consumer demand for mobile IV therapy continues to rise as individuals prioritize convenience and personalized wellness care. However, this growing market does not change the legal requirements. Even in mobile or concierge settings, a licensed provider must perform the infusion under appropriate medical authorization.
For those considering non-traditional career paths in IV therapy, the legal boundaries are clear: proper licensure, clinical training, and physician oversight remain non-negotiable across virtually every state. Understanding how clinic and home settings differ further clarifies provider requirements.
What Is the Difference Between IV Therapy in Clinics and at Home?
The difference between IV therapy in clinics and at home comes down to setting, staffing structure, and oversight level. Clinic settings operate under institutional protocols, while mobile services bring licensed professionals directly to clients.
Who Administers IV Therapy in Hospital and Clinic Settings?
IV therapy in hospital and clinic settings is administered by licensed healthcare professionals, including registered nurses, licensed practical nurses, and nurse practitioners, who operate under direct institutional oversight. Alabama’s administrative code requires that the minimum preparation for an LPN to perform IV therapy includes successful completion of an organized program of study and supervised clinical practice. Clinics maintain on-site medical teams, standardized equipment, and established emergency protocols.
Despite this structured environment, compliance gaps still emerge. Disciplinary records from Iowa revealed an investigation into a nurse sanctioned for professional incompetence due to allegations tied to IV therapy clinic operations. These cases underscore why IV therapy requires a standardized safety framework, regardless of the setting. For patients receiving treatment in a clinic, verifying that the facility follows state-specific staffing and supervision requirements remains essential.
Who Administers IV Therapy in Mobile and At-Home Settings?
IV therapy in mobile and at-home settings is administered by licensed registered nurses or nurse practitioners who travel to the client’s location. These professionals carry the same clinical credentials as their hospital counterparts but deliver care in homes, offices, or event venues.
This convenience-driven model is expanding rapidly. According to a 2024 Nova One Advisor report, the U.S. mobile IV hydration therapy market was valued at USD 568.25 million and is projected to reach approximately USD 1,556.29 million by 2034. Consumer demand continues to rise as individuals prioritize personalized wellness and on-demand medical concierge services. Mobile providers now offer treatments ranging from immunity boosters to comprehensive wellness drips.
The key distinction is not provider quality; it is accessibility. Choosing a mobile IV therapy provider with verified nursing credentials ensures the same standard of care delivered outside traditional clinical walls.
What Should You Look for When Choosing an IV Therapy Provider?
When choosing an IV therapy provider, you should verify credentials, confirm professional nursing staff, and evaluate safety protocols. The following sections cover each of these critical factors.
How Do You Verify a Provider’s Credentials and Licensing?
You verify a provider’s credentials and licensing by confirming that every clinician holds an active, unrestricted license issued by your state’s nursing or medical board. Most state boards maintain online license lookup tools where you can check a provider’s status, disciplinary history, and scope-of-practice authorization in minutes.
Key credentials to verify include:
- A current registered nurse (RN) or advanced practice license with no restrictions or sanctions.
- State-specific IV therapy certification, which many states require before a nurse can legally administer infusions.
- Specialty credentials such as the CRNI or VA-BC designation, which demonstrate advanced infusion competency.
- A valid medical order from a licensed provider with prescriptive authority, confirming that treatments are physician-supervised.
Any provider unwilling to share license details or facility documentation should be considered a red flag.
Why Does Professional Nursing Staff Matter for IV Therapy?
Professional nursing staff matter for IV therapy because nurses possess the clinical training to assess patients, identify adverse reactions, and respond to emergencies during infusion. IV catheter insertion requires practiced technique; improperly placed lines increase the risk of infiltration, phlebitis, and infection.
According to REVIV Wellness, expert medical professionals emphasize that IV therapy carries significant clinical risks and requires a standardized global safety framework similar to those used for vaccines and other medications. Registered nurses complete extensive clinical hours covering vascular access, pharmacology, and patient monitoring. This depth of education enables them to recognize subtle complications, such as changes in skin temperature or swelling at the insertion site, before they escalate. For any provider you consider, confirming that licensed nurses perform every infusion is one of the most important steps you can take.
What Safety Protocols Should a Qualified Provider Follow?
The safety protocols a qualified provider should follow include standardized procedures for sterile technique, patient screening, adverse event response, and proper medication handling. Without these safeguards, even routine infusions carry preventable risks.
Essential safety protocols include:
- A pre-infusion health assessment covering allergies, medications, and medical history.
- Aseptic technique for catheter insertion, including proper hand hygiene, skin antisepsis, and sterile supplies.
- Continuous patient monitoring throughout the session for signs of infiltration, phlebitis, or allergic reaction.
- Emergency preparedness with anaphylaxis kits, oxygen, and clear escalation procedures.
- Proper documentation of every treatment, including lot numbers, dosages, and patient vitals.
According to the National Association of Boards of Pharmacy (NABP), regulators from the NABP, FSMB, and NCSBN have convened to address safety concerns in IV hydration clinics following reports of serious adverse events and a lack of national standards for these facilities. This regulatory gap makes individual provider vetting even more critical.
With a clear framework for evaluating providers, the next step is understanding how nurse-administered mobile IV therapy works in practice.

How Does Nurse-Administered Mobile IV Therapy Work?
Nurse-administered mobile IV therapy works by sending licensed registered nurses directly to a client’s location to perform intravenous infusions. The following sections cover how The Drip IV Infusion delivers this service and what to remember about proper IV administration.
Can The Drip IV Infusion’s Registered Nurses Deliver IV Therapy at Your Home?
Yes, The Drip IV Infusion’s registered nurses can deliver IV therapy at your home. Founded in Fall 2022 by professionals with decades of experience in nursing, emergency medicine, and IV medical techniques, The Drip IV Infusion sends licensed RNs directly to homes and workplaces across Arizona. Each session typically takes one hour and includes personalized IV cocktails, specialty treatments, and customizable add-ons.
Registered nurses are permitted to administer IV therapy under the supervision of a licensed physician or nurse practitioner, provided they have demonstrated clinical competency. This home-based model reflects a rapidly expanding industry; according to a 2025 report from Yahoo Finance, the U.S. home infusion therapy market was estimated at USD 21.95 billion, with a projected compound annual growth rate of 7.7%.
The Drip IV Infusion combines this growing demand for convenience with professional nursing expertise, ensuring clients receive safe, effective infusions without leaving their preferred setting.
What Should You Remember About Who Can Administer IV Therapy?
What you should remember about who can administer IV therapy comes down to three essential points:
- Only licensed healthcare professionals, such as registered nurses, nurse practitioners, physician assistants, and physicians, are legally authorized to administer IV therapy.
- Scope-of-practice laws vary by state, so the specific qualifications, supervision requirements, and certifications a provider needs depend on local regulations.
- Verifying credentials before any infusion session protects your safety, since IV therapy carries clinical risks that require trained, competent professionals.
For those choosing a mobile service, working with a provider that employs experienced registered nurses is the most practical way to ensure both legal compliance and clinical quality. The Drip IV Infusion staffs every appointment with skilled RNs who bring professional-grade care to wherever you are.


